Which States Could Be Hit Hardest By Reductions in Federal Medicaid Spending and Per Capita Caps?
A new issue brief from the Kaiser Family Foundation examines the factors that could affect states’ ability to cope with reductions in federal Medicaid funding of the sort proposed in the House-passed American Health Care Act (AHCA). The bill would eliminate enhanced federal matching funds for the Affordable Care Act’s Medicaid expansion and convert Medicaid to a per capita cap or block grant system of financing.
The analysis looked at 30 risk factors in five key areas that would affect states’ ability to cope with federal Medicaid funding reductions. Factors include the age, health needs, and relative wealth of their populations; the robustness of their existing Medicaid programs; the conditions and costliness of their health care markets; and their fiscal capacity to ramp up state spending and revenues.
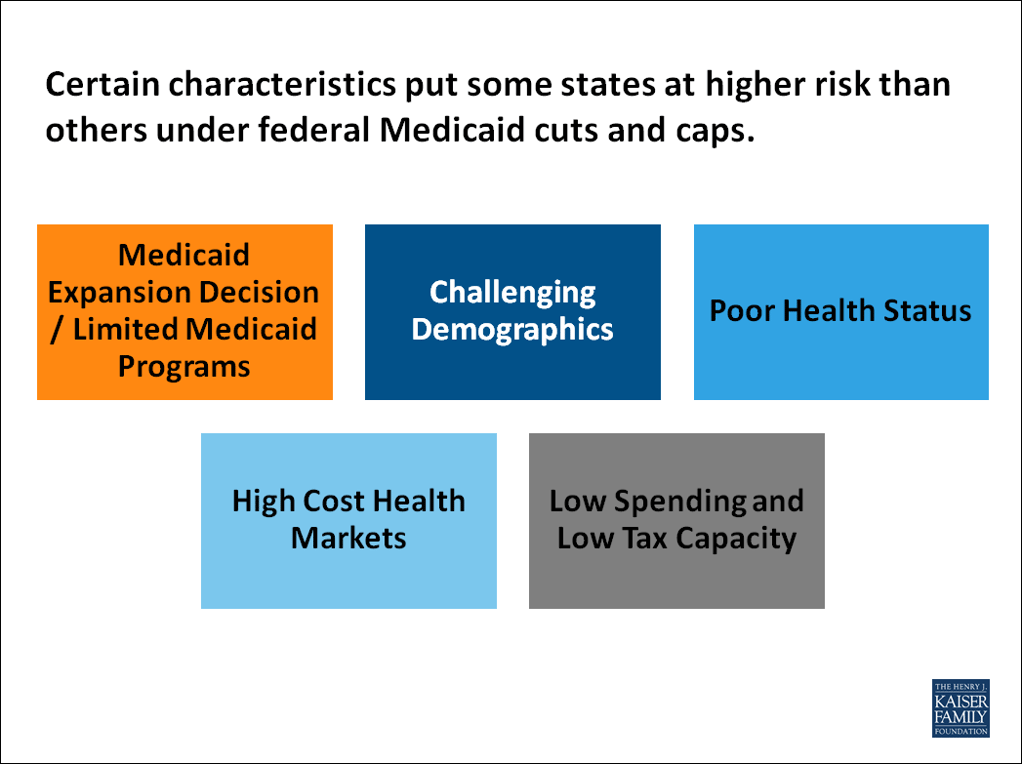
For example, state Medicaid programs that have limited benefits or low provider reimbursement rates would be less able to respond to new cost pressures by paring back benefits or trimming rates. At the same time, states with aging populations, relatively high levels of residents with disabilities, more areas with health professional shortages, and higher shares of low-income residents may have higher demand for Medicaid services than other states, but less capacity to fill in federal funding gaps with state dollars. The analysis finds that all states could face challenges in responding to federal Medicaid cuts and caps to varying degrees, but more than 6 in 10 states rank in the top five for more than one factor. Eleven states rank highest (in the top five) in five or more of these risk categories: Alabama, Arizona, Florida, Georgia, Kentucky, Louisiana, Mississippi, New Mexico, South Carolina, Texas, and West Virginia.
The analysis also examines which states could be hardest hit by a rollback in funding for the ACA Medicaid expansion. Among the 32 states that have expanded Medicaid, those arguably with the most to lose include Arkansas, Kentucky, Oregon, and Nevada, the analysis finds. They rank high among states with a combination of the largest coverage gains under the Medicaid expansion, as well as the highest shares of Medicaid expansion enrollees, and federal expansion funding as a share of total Medicaid spending – combinations which make them more vulnerable to significant disruption if enhanced federal funding ends.
The new brief includes tables with state-level data for each of the 30 risk factors considered in the analysis.

Filling the need for trusted information on national health issues, the Kaiser Family Foundation is a nonprofit organization based in Menlo Park, California.
